
Rajiv was 56 years old, a retired schoolteacher from Delhi, and someone who had never spent a night in a hospital in his life. One morning, he woke up coughing, as he sometimes did. But this time, when he looked into his handkerchief, there was blood. Not a lot. A small streak, pink against the white fabric. He stared at it for a long time. He told himself it was probably nothing. Maybe he had bitten his cheek during the night. Maybe it was a burst blood vessel from coughing too hard. He folded the handkerchief and set it aside.
Three weeks later, he was sitting in my clinic at Artemis Hospital, having just been diagnosed with Stage 2 non-small cell lung cancer. That small streak of pink had been the first sign. And what Rajiv did not know, and what most people never know, is that coughing up blood is never something to put aside and wait on. It is the kind of symptom that demands an answer.
If you or someone you love has seen blood while coughing, this article will tell you exactly what it means, when it is serious, and what steps to take. No alarm, no panic. Just the facts you need to make the right call.
What is hemoptysis? Hemoptysis is the act of coughing up blood or blood-stained mucus from the airways or lungs. It is different from blood that comes from the mouth, throat, nose, or stomach. The blood originates below the vocal cords, from the bronchi, airways, or lung tissue itself. |
Here is the surprising truth about hemoptysis: it is far more common than most people realize, and it is responsible for a significant number of hospital visits every year. According to a review published in PMC, hemoptysis accounts for 6.8% of all outpatient pulmonary clinic visits and 11% of all admissions to hospital pulmonary services in the United States. In 2016 alone, over 8,240 hospitalizations in the US were directly attributed to hemoptysis.
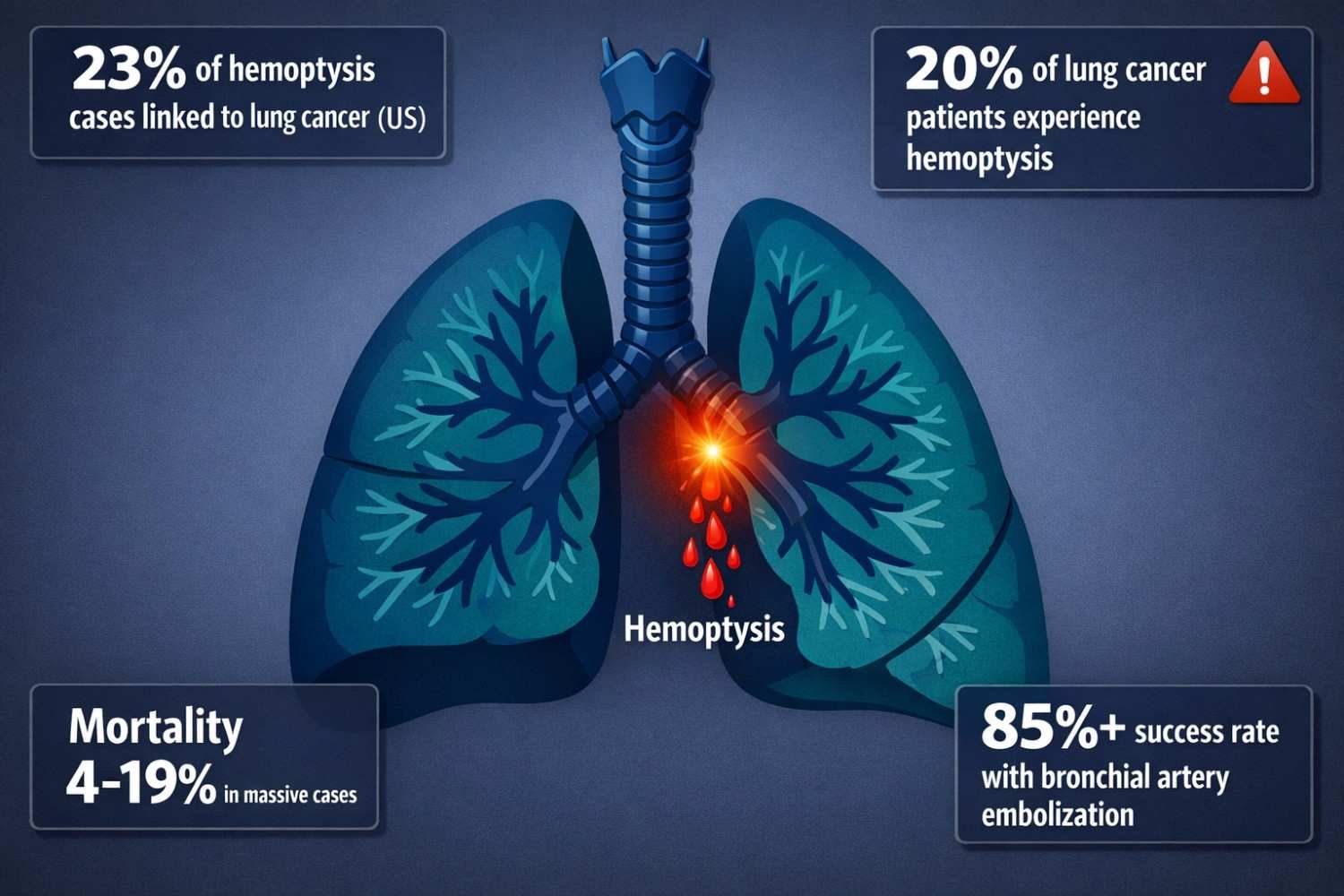
What makes hemoptysis so clinically significant is what lies behind it. In the US, lung cancer accounts for approximately 23% of all hemoptysis cases, making it the third most common cause. And roughly 20% of all lung cancer patients will experience hemoptysis at some point during their illness, according to research from MyLungCancerTeam. For some, it is the very first symptom that leads to diagnosis.
Not all cases of coughing up blood carry the same level of urgency. Doctors classify hemoptysis into three categories based on the volume of blood:
| Category | Blood Volume in 24 Hours | Urgency Level | What It Means |
| Minor (Mild) | Less than a teaspoon (a few streaks) | See a doctor within 24 to 48 hours | Infection, bronchitis, or early-stage cancer |
| Moderate | A few teaspoons to less than 200 ml | Same-day medical evaluation needed | Structural lung disease, tumor involvement |
| Massive | More than 200 ml (about a cup or more) | Emergency, call 112 or go to ER immediately | Life-threatening airway obstruction possible |
What most people do not realize is that the amount of blood is not a reliable indicator of how serious the underlying cause is. A small streak of blood could be the first sign of a lung tumor. A larger bleed could be from a treatable infection. The only way to know for certain is a proper medical evaluation.
Noticed blood in your cough? Do not wait and watch. Book a consultation with Dr. Parveen Yadav at Artemis Hospital Gurgaon today: chestsurgeryindia.com/contact |
The causes of hemoptysis range from minor and self-limiting to serious and life-threatening. Understanding the full list matters because the source of the bleed, not just the amount, determines what comes next.
| Cause | How Common | Key Features |
| Bronchitis (acute or chronic) | Most common in outpatient settings | Blood-streaked mucus, persistent cough, usually clears with treatment |
| Tuberculosis (TB) | Leading cause globally, especially in India | Night sweats, weight loss, prolonged cough with blood |
| Bronchiectasis | About 20% of hospital cases | Recurrent lung infections, widened damaged airways |
| Lung Cancer | 23% of US cases, rising in India | May be only symptom at first; requires urgent workup |
| Pneumonia | Common in hospitalized patients | Fever, chills, rust-colored or blood-tinged sputum |
| Pulmonary Embolism | Rare but life-threatening | Sudden chest pain, breathlessness, blood clot in lung |
| Fungal Infections (Aspergillosis) | Rare but serious in immunocompromised | History of immune disease or steroid use |
| Mitral Valve Disease | Cardiovascular cause | Pink frothy sputum, heart disease history |
In India, the picture is different from Western data. Tuberculosis remains the single most common cause of hemoptysis globally, and given India's TB burden, any patient presenting with blood-stained sputum must be evaluated for TB alongside other causes. However, a growing and underappreciated factor is the rise of lung cancer in non-smokers, particularly in women exposed to biomass fuel smoke and urban air pollution. As an oncologist in Gurgaon, I regularly see patients who dismissed their cough and blood as a TB symptom, delaying a lung cancer diagnosis by months.
The appearance of the blood you cough up can offer useful clues. Here is what to observe and report to your doctor:
• Bright red, frothy blood: likely from the lungs or airways, classic hemoptysis
• Pink or blood-streaked mucus: smaller bleed, possibly early-stage or infection-related
• Rust-colored or brown sputum: older blood mixed with mucus, common in pneumonia
• Dark red, coffee-ground appearance: likely from the stomach (hematemesis), not the lungs
• Clotted blood with no mucus: may suggest a vascular source, needs urgent evaluation
Bright red frothy blood is the clearest sign of true hemoptysis. Coffee-ground or dark material that comes up with nausea is more likely from the digestive system. The distinction matters because treatment paths are completely different.
What most people do not realize is that even a single episode of blood in your cough deserves medical attention if it is unexplained. The following situations require immediate action:
Go to the Emergency Room Immediately If You Experience: Coughing up more than a few teaspoons of blood in a single episode / Blood that keeps coming back over several days / Coughing blood with chest pain or severe breathlessness / Dizziness, fainting, or a rapid drop in blood pressure alongside the bleeding / A known history of lung cancer and sudden increase in blood volume |
For reference: a study from Archivos de Bronconeumologia found that advancing age from 40 years, former airway cancer history, and abnormal chest X-ray findings are the strongest predictors of malignancy in hemoptysis patients. Crucially, the study also showed that smoking status alone did not reliably separate lung cancer cases from non-cancer cases in hemoptysis patients. Non-smokers with hemoptysis also developed lung cancer. This means every hemoptysis patient, smoker or not, deserves a thorough workup.
Here is something that almost no general health article mentions. In the context of lung cancer and large blood vessel involvement, there is a clinical phenomenon called the sentinel bleed. This is a small episode of hemoptysis that occurs before a much larger, potentially life-threatening bleed. According to PMC research on hemoptysis in malignancy, most cases of massive hemoptysis occur after a prior history of smaller bleeds that were not investigated or were dismissed.
This is exactly why a small streak of blood in a cough is never 'nothing to worry about.' It could be your body's first warning before a more serious event. Treating the sentinel bleed as a trigger for urgent evaluation can be life-saving.
Of all the causes of hemoptysis, lung cancer deserves special attention because it is both serious and treatable when caught early. According to research published in PMC on cancer-related hemoptysis, hemoptysis in lung cancer occurs through several different mechanisms:
• Tumor neovascularization: growing tumors develop their own blood supply network, which is fragile and prone to bleeding
• Tumor surface exfoliation: as outer layers of the tumor break down, they bleed into the airway
• Vessel erosion: tumors that grow near blood vessels can erode through the vessel wall, causing bleeding directly into the airway
• Tumor necrosis: when tumor tissue dies due to rapid growth, the dying cells release blood
• Post-procedure bleeding: bronchoscopy or biopsy for lung cancer diagnosis can sometimes trigger a brief bleed
In about 27% of all hemoptysis cases, lung cancer is the underlying cause. For patients with non-small cell lung cancer (NSCLC), 52% of bleeds trace back to damage in the bronchial arteries, according to a European Respiratory Journal study cited by MyLungCancerTeam. In severe cases, bronchial artery involvement rises to 82%.
This is one of the most common questions I hear in my clinic, and the answer surprises most patients. The volume of blood coughed up does not predict the stage of lung cancer. According to Healthline's medically reviewed guide, you can cough up blood at any stage of lung cancer, from Stage 1 to Stage 4. A small streak of blood at Stage 1 can be far more treatable than a larger bleed at Stage 3. Only a CT scan, bronchoscopy, and biopsy can determine the actual stage and guide treatment.
Concerned about blood in your cough? Get a specialist opinion. Reach out to Chest Surgery India for a thoracic evaluation with Dr. Parveen Yadav: chestsurgeryindia.com/lung-cancer-treatment |
When you present with hemoptysis, any thoracic specialist will follow a structured diagnostic pathway. Here is what that process looks like, step by step, so you know what to expect:
| Step | Investigation | What It Looks For |
| Step 1 | Medical history and physical exam | Duration, frequency, blood volume, associated symptoms, smoking history, TB exposure |
| Step 2 | Chest X-ray | Visible masses, infiltrates, cavities, or abnormal lung markings (75% sensitivity for lung cancer) |
| Step 3 | CT scan of the chest | Detailed mapping of tumors, vessels, lymph nodes, and airway structure |
| Step 4 | Bronchoscopy | Direct visual inspection of airways; identifies bleed source and allows biopsy if a mass is seen |
| Step 5 | Sputum cytology | Checks coughed-up mucus for cancer cells |
| Step 6 | PET scan (if cancer suspected) | Shows metabolic activity of tumors and checks for spread |
| Step 7 | Molecular/genetic testing | Identifies EGFR, ALK, ROS1 mutations to guide targeted therapy |
The most critical point about diagnosis: chest X-ray is not enough on its own. Early lung tumors can be invisible on a plain X-ray but clearly visible on a CT scan. If you are over 40 and have unexplained hemoptysis, insist on a CT scan of the chest if your doctor has not ordered one. This is especially important for patients in Delhi-NCR given the region's high ambient air pollution levels.
When the bleed is mild and the underlying cause is identified, treatment is focused on addressing that cause directly. Here are the most common treatment approaches:
• Antibiotics or antifungals: for hemoptysis caused by infection, TB, or fungal disease
• Cough suppressants: to reduce the mechanical irritation that worsens airway bleeding
• Bronchoscopic intervention: the bronchoscope can be used to apply heat (cauterize), freeze (cryotherapy), or inject agents directly to seal a bleeding point
• Radiation therapy: for cancer-related hemoptysis, targeted radiation can shrink the tumor and stop bleeding from inside the airway
• Targeted therapy and immunotherapy: for EGFR-mutant or other mutation-driven lung cancers, systemic therapy that shrinks the tumor is the most effective way to stop the bleeding at its source
Massive hemoptysis, defined as losing more than 200 ml of blood in 24 hours, carries a mortality rate of 4 to 19% without prompt intervention, according to studies reviewed by Lung Cancer Center. The immediate priority is protecting the airway from obstruction by blood. Here is how massive hemoptysis is managed:
• Endotracheal intubation: a breathing tube is inserted to keep the airway open and prevent blood from flooding the other lung
• Bronchoscopy for localization and tamponade: the bleed site is identified and a balloon catheter can be used to temporarily block the bleeding airway
• Bronchial artery embolization (BAE): a catheter is threaded through the artery supplying the bleeding area and a blocking agent is injected to cut off blood flow to the bleed site. This is now the gold standard for emergency hemoptysis control
• Surgical resection: in select cases where BAE is not possible or has failed, emergency surgical removal of the bleeding lung segment is performed. This is rare but sometimes the only option to save a patient's life
The good news is that bronchial artery embolization has a technical success rate of over 85% in stopping acute massive hemoptysis, making surgery rarely necessary as a primary response.
Beyond the physical, coughing up blood causes a level of fear and anxiety that is significant and often undertreated. Research cited in PMC's cancer hemoptysis review notes that hemoptysis causes considerable emotional and psychological distress in both patients and their families, and that palliative care and psychological support are recognized components of comprehensive hemoptysis management.
In my experience, patients who understand what is happening and why are far less likely to delay seeking care or to fall into panic-driven decision-making. Knowing the facts, like what the blood color means, what tests to expect, and what treatments exist, transforms fear into preparedness. And preparedness saves lives.
If your hemoptysis is traced to lung cancer, the next step is a structured, multidisciplinary treatment plan. As a lung cancer specialist in Gurgaon, my team follows a precise pathway to give every patient the best possible outcome:
• Staging with CT and PET scan: determines how far the cancer has spread before any treatment begins
• Molecular profile testing: checks for EGFR, ALK, ROS1, and other actionable mutations
• Tumor board review: thoracic surgeon, medical oncologist, radiation oncologist, and pathologist review the case together before deciding treatment
• Robotic-assisted VATS surgery: for early-stage lung cancer, minimally invasive robotic surgery using the Da Vinci Xi system offers precise tumor removal with smaller incisions and faster recovery
• Targeted therapy: for mutation-driven cancers, oral targeted drugs can shrink tumors faster than standard chemotherapy
• Immunotherapy: for cancers with high PD-L1 expression, immunotherapy has significantly improved long-term survival rates
The 5-year survival rate for early-stage lung cancer when caught and treated promptly is approximately 59%, compared to just 6% at the late stage, according to the American Lung Association's 2020 report. That gap is why every streak of blood in a cough deserves urgent attention, not a wait-and-see approach.
| Situation | What To Do | Timeline |
| Single small streak, no other symptoms | Call your doctor and book an appointment | Within 24 to 48 hours |
| Recurring streaks over 2 or more days | See a doctor the same day, ask for a chest CT | Same day |
| Blood with chest pain or breathlessness | Go to the emergency room immediately | Right now |
| Large amount of blood (a cup or more) | Call emergency services (112). This is life-threatening | Immediately |
| Blood + known lung cancer history | Contact your oncologist or ER without delay | Immediately |
| Blood + weight loss + night sweats | Same-day evaluation, rule out TB and lung cancer | Same day |
Do not let fear delay the care you need. Call Dr. Parveen Yadav's clinic directly at +91 9540210956 or request a consultation online: chestsurgeryindia.com/contact |
Here is a quick summary of the most important points from this guide:
• Hemoptysis is never normal. Any unexplained blood in a cough needs medical evaluation, regardless of the volume
• Lung cancer causes about 23% of all hemoptysis cases in the US, and is a growing cause in India among non-smokers
• The amount of blood does not indicate the cancer stage. Even a small streak can be an early warning that is entirely treatable
• The sentinel bleed is real. Small bleeds that precede large ones are missed warning signs that can cost lives if ignored
• CT scan is more reliable than a chest X-ray for detecting early tumors in hemoptysis workup
• Early-stage lung cancer has a 59% five-year survival rate. Catching it at the first symptom makes all the difference
• Bronchial artery embolization has over 85% success in stopping massive hemoptysis without surgery
• Targeted therapy and immunotherapy are highly effective for specific mutation-driven lung cancers linked to hemoptysis
Rajiv, the retired schoolteacher from the beginning of this story, completed robotic-assisted surgery and targeted therapy at our center. Today, 14 months later, his scans are clear. He told me recently that he almost did not come to the clinic because he thought the blood was 'too small to matter.' It was not.
The question I want to leave you with is this: if the person sitting next to you right now coughed into a tissue and saw a streak of red, would they know what to do next? Share this article so they do.

18+ Yrs Exp | 5,700+ Thoracic & Robotic Cancer Surgeries
Dr. Parveen Yadav is a Director and Senior Consultant in Thoracic and Surgical Oncology, specializing in minimally invasive and robotic lung and esophageal surgeries, with advanced training from AIIMS and Tata Memorial Hospital.
View Full Profile Best Bronchopleural Fistula Treatment in Gurgaon: What to Look for in a Thoracic Surgeon
Best Bronchopleural Fistula Treatment in Gurgaon: What to Look for in a Thoracic Surgeon
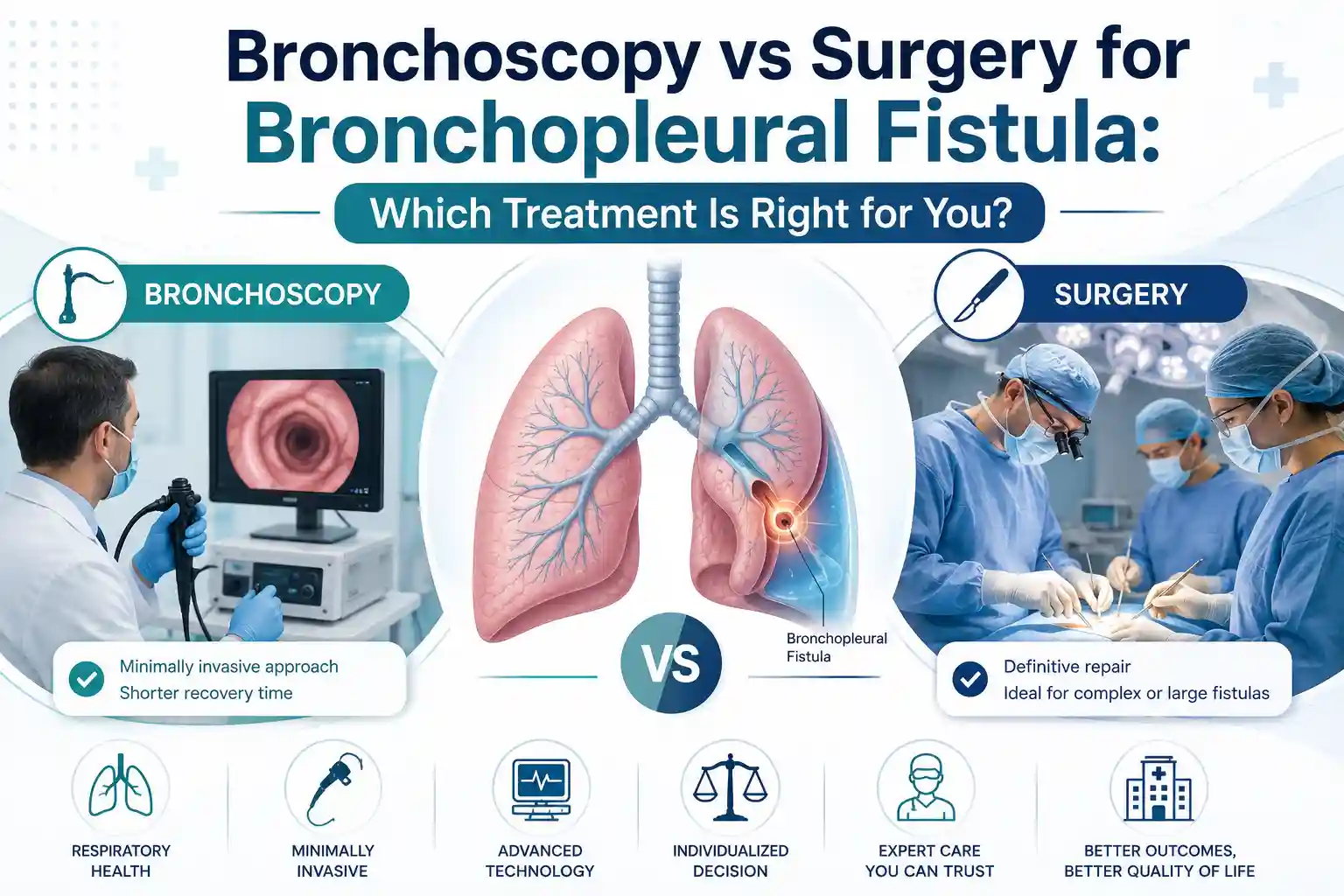 Bronchoscopy vs Surgery for Bronchopleural Fistula: Which Treatment Is Right for You?
Bronchoscopy vs Surgery for Bronchopleural Fistula: Which Treatment Is Right for You?
 Lung Cancer in Non-Smokers: Symptoms, Causes and When to See a Specialist
Lung Cancer in Non-Smokers: Symptoms, Causes and When to See a Specialist
Choosing the best bronchopleural fistula treatment in Gurgaon? Here is what to look for in a thoracic surgeon, hospital, and care team before you decide.
Bronchoscopy or surgery for bronchopleural fistula? Compare both options, success rates, recovery, and costs. Expert guidance from Dr. Parveen Yadav, Gurgaon.
Know the symptoms, causes, risk factors, and warning signs of lung cancer in non-smokers. Learn when to consult a lung cancer specialist in Gurgaon.
Copyright 2026 © Dr .Parveen Yadav all rights reserved.
Proudly Scaled by Public Media Solution!