

Tracheal cancer, though relatively rare, is a condition that demands attention and understanding. Often shrouded in misconceptions, separating myths from facts is crucial for awareness and effective management. Let's delve into nine common myths and facts surrounding tracheal cancer.
Fact: While smoking is a significant risk factor, tracheal cancer can affect non-smokers too. Exposure to environmental toxins or radiation, genetic predisposition, and certain infections can also contribute to its development.
It is known that smoking is a significant risk factor for tracheal cancer. However, it is essential to note that even non-smokers can develop this condition. Exposure to environmental toxins, radiation, genetic factors, and infections can increase the likelihood of developing tracheal cancer.
Therefore, it's crucial not to attribute the disease solely to smoking but to consider various factors that could contribute to its development in both smokers and non-smokers.
Fact: Symptoms such as persistent cough, wheezing, or hoarseness may indicate tracheal cancer. However, early-stage tracheal cancer often exhibits no symptoms, making regular screenings crucial, especially for individuals with risk factors.
While symptoms like chronic cough, wheezing, hoarseness, and difficulty breathing are commonly associated with tracheal cancer, it's important to note that not all cases present with obvious symptoms, particularly in the early stages. Some individuals may experience no symptoms, leading to delayed diagnosis and treatment. Therefore, regular screenings and awareness of risk factors are essential for detecting tracheal cancer early when treatment is most effective.
Latest Blog: Exploring Tracheal Cancer: Causes, Symptoms, and Risk Factors
Fact: Early diagnosis and appropriate treatment significantly improve prognosis. Surgical intervention, radiation therapy, and chemotherapy are among the treatment modalities that offer hope for patients with tracheal cancer, enhancing survival rates and quality of life.
While tracheal cancer can be aggressive and challenging to treat, it's not always fatal. Early diagnosis and prompt treatment significantly improve the prognosis for individuals with this disease. Tracheal cancer can be managed effectively through various treatment options, including surgery, radiation therapy, chemotherapy, and targeted therapy. These treatments can improve survival rates. With advancements in medical technology and treatment approaches, many individuals diagnosed with tracheal cancer can achieve remission and lead fulfilling lives.
Fact: Surgery is the primary method for treating tumours, but the treatment plan may vary depending on the tumour's size and location. A mixture of chemotherapy and radiation therapy can be used alongside surgery to enhance its efficacy.
Surgery is often the primary treatment for tracheal cancer, particularly for early-stage tumours. The treatment approach for tracheal cancer may vary depending on factors such as cancer size, location, stage, patient's overall health, and personal preferences.
Radiation therapy or chemotherapy can be used alone or in combination with surgery to manage tracheal cancer effectively. Therefore, patients must discuss all available treatment options with their healthcare team to determine the most suitable approach for their case.
Fact: Tracheal cancer is not contagious. It does not spread through casual contact, making it essential to dispel misconceptions that may stigmatise affected individuals.
Tracheal cancer is a non-communicable disease, meaning it cannot be transmitted from person to person through casual contact. Unlike infectious diseases caused by bacteria, viruses, or other pathogens, tracheal cancer develops due to genetic mutations or environmental factors and cannot be spread to others. Therefore, it's crucial to educate the public and dispel any misconceptions that may lead to stigma or discrimination against individuals diagnosed with tracheal cancer.
Fact: Tracheal cancer can occur at any age, although it is more common among older adults. Awareness of risk factors and early symptoms is crucial for prompt diagnosis and management across all age groups.
Tracheal cancer can occur at any age but is more commonly diagnosed in adults over 60. Various factors, such as smoking, exposure to environmental toxins, genetic predisposition, and certain medical conditions, can increase the risk of developing tracheal cancer in individuals of all ages.
Fact: Leading a healthy lifestyle, including quitting smoking, avoiding environmental toxins, and eating a balanced diet, can decrease the risk of tracheal cancer and improve overall health.
Tracheal cancer can be caused by various factors like genetic predisposition and environmental exposures that are beyond individual control. Selecting a healthy lifestyle can effectively reduce the risk of developing this disease.
To prevent tracheal cancer, it is essential to quit smoking, avoid exposure to environmental carcinogens like asbestos and radon, maintain a healthy weight, and eat fresh fruits and vegetables. Therefore, promoting healthy lifestyle habits is crucial in preventing tracheal cancer.
Fact: Treatment plans are tailored to individual cases, considering factors like the cancer stage and the patient's overall health. Sometimes, a watchful waiting approach may be appropriate, especially for slow-growing tumours.
While tracheal cancer can be aggressive and may require aggressive treatment, such as surgery, radiation therapy, or chemotherapy, the treatment approach is not one-size-fits-all. Treatment plans are tailored to individual cases, taking into account factors such as the stage and location of the tumour, the patient's overall health and preferences, and the potential benefits and risks of treatment.
In some instances, particularly for slow-growing tumours or when the patient's health precludes aggressive intervention, a watchful waiting approach may be appropriate, closely monitoring the tumour's progression over time. It is highly recommended that patients thoroughly discuss all possible treatment options with their healthcare team before deciding. This will help patients make informed decisions appropriate to their needs.
Fact: While some risk factors for tracheal cancer are beyond control, adopting preventive measures such as smoking cessation and minimising exposure to environmental toxins can reduce the risk. Regular screenings also aid in early detection and timely intervention.
While it's not possible to prevent all cases of tracheal cancer, adopting preventive measures can help reduce the risk of developing this disease. Quitting smoking, avoiding exposure to environmental carcinogens like asbestos and radon, maintaining a healthy lifestyle, and participating in regular screenings can lower the risk of tracheal cancer and facilitate early detection and intervention when necessary. Therefore, promoting awareness of risk factors and encouraging preventive measures are essential to tracheal cancer prevention efforts.
In conclusion, debunking myths surrounding tracheal cancer is essential for raising awareness, promoting early detection, and improving outcomes for affected individuals. By understanding the facts and addressing misconceptions, we can support those impacted by this condition and work towards better outcomes.
Dr. Parveen Yadav and Chest Surgery India offer comprehensive care and expertise for individuals seeking tracheal cancer treatment or surgery in Gurgaon or Delhi. Dr. Yadav is renowned as the best doctor for tracheal cancer and a specialist in the field, ensuring patients receive personalised treatment at the best tracheal cancer hospital in the region.
1. Is tracheal cancer always fatal?
Ans: No, tracheal cancer isn't always fatal. Early diagnosis and appropriate treatment significantly improve prognosis, enhancing survival rates and quality of life.
2. Can lifestyle changes reduce the risk of tracheal cancer?
Ans: Yes, leading a healthy lifestyle, including quitting smoking, avoiding environmental toxins, and maintaining a balanced diet, can decrease the risk of tracheal cancer.
3. Is tracheal cancer contagious?
Ans: No, tracheal cancer is not contagious. It does not spread through casual contact as it develops due to genetic mutations or environmental factors.
4. What are the treatment options for tracheal cancer?
Ans: Treatment options include surgery, radiation therapy, chemotherapy, and targeted therapy. The choice depends on factors such as cancer stage, location, and the patient's overall health.
5. At what age can one develop tracheal cancer?
Ans: Tracheal cancer can occur at any age, but it's more common in older adults. However, individuals of all ages should be aware of risk factors and symptoms for timely diagnosis and management.
Dr. Parveen Yadav is a highly recommended surgeon or specialist for Tracheal cancer treatment in Gurgaon, Delhi. He specialises in minimally invasive and robotic thoracic onco surgery. He has been recognised for 17+ years as the best chest surgeon in Gurgaon, Delhi, for his expertise in treating chest-related (chest surgery) ailments, such as Esophageal, Lung, Tracheal (Throat), Chest wall tumours, Mediastinal Tumors, Empyema, and Bronchopleural Fistula cancer. With a focus on precision and innovation, he is dedicated to offering exceptional care to his patients, utilising advanced techniques to ensure optimal outcomes.

18+ Yrs Exp | 5,700+ Thoracic & Robotic Cancer Surgeries
Dr. Parveen Yadav is a Director and Senior Consultant in Thoracic and Surgical Oncology, specializing in minimally invasive and robotic lung and esophageal surgeries, with advanced training from AIIMS and Tata Memorial Hospital.
View Full Profile Robotic Surgery for Esophageal Cancer in India: Benefits, Recovery and When It Is Recommended
Robotic Surgery for Esophageal Cancer in India: Benefits, Recovery and When It Is Recommended
 Best Bronchopleural Fistula Treatment in Gurgaon: What to Look for in a Thoracic Surgeon
Best Bronchopleural Fistula Treatment in Gurgaon: What to Look for in a Thoracic Surgeon
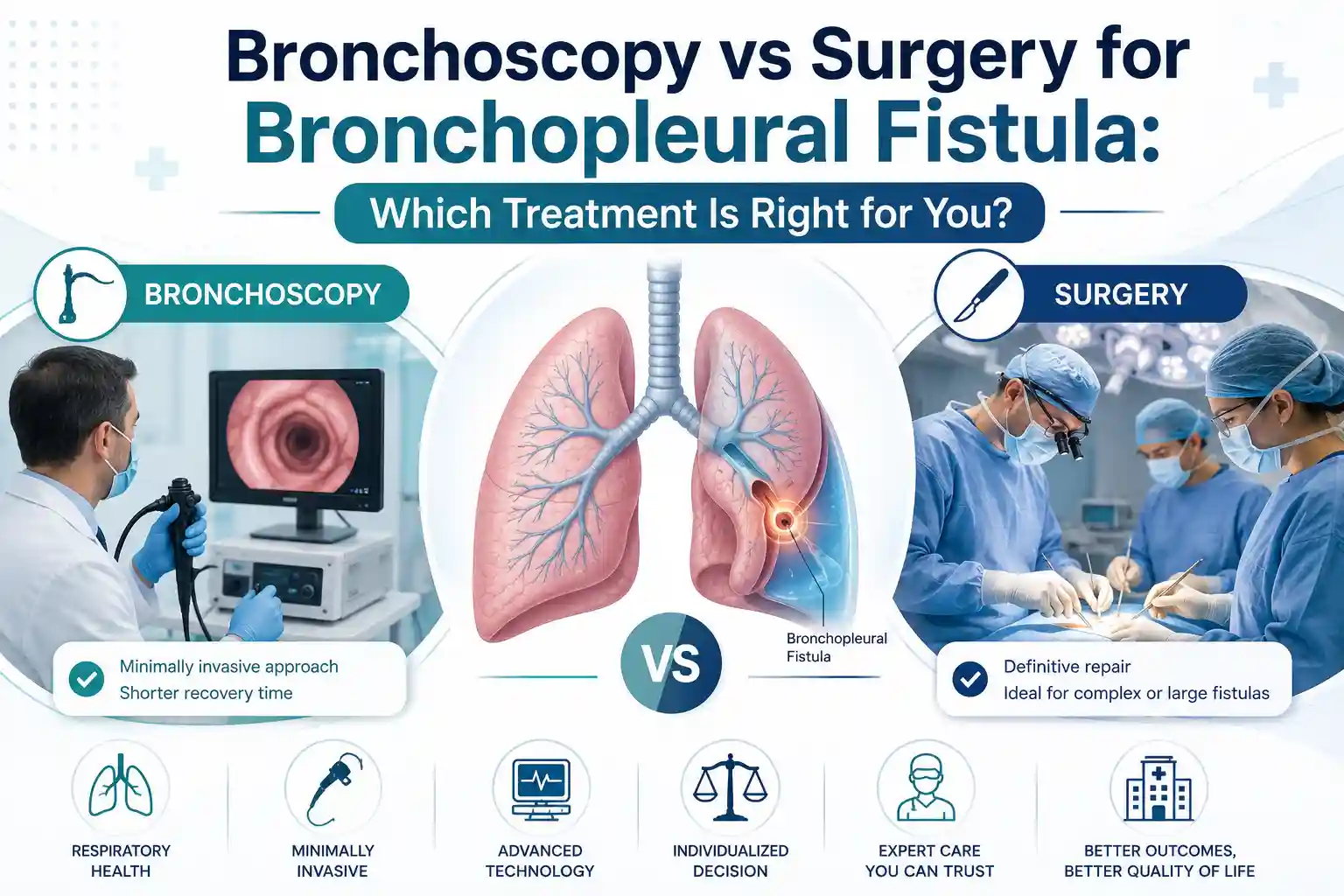 Bronchoscopy vs Surgery for Bronchopleural Fistula: Which Treatment Is Right for You?
Bronchoscopy vs Surgery for Bronchopleural Fistula: Which Treatment Is Right for You?
Learn when robotic surgery for esophageal cancer in India is recommended, its benefits, recovery, and how to consult an expert in Gurgaon.
Choosing the best bronchopleural fistula treatment in Gurgaon? Here is what to look for in a thoracic surgeon, hospital, and care team before you decide.
Bronchoscopy or surgery for bronchopleural fistula? Compare both options, success rates, recovery, and costs. Expert guidance from Dr. Parveen Yadav, Gurgaon.
Copyright 2026 © Dr .Parveen Yadav all rights reserved.
Proudly Scaled by Public Media Solution!