

Cancer, in any form, is extremely dangerous for patients. It not only hampers the production of healthy cells but also mutates them while multiplying their numbers in your body. While all cancers are catastrophic, the ones that are not easy to diagnose are the worst.
Esophageal cancer is one such disease that is not diagnosed readily. Patients often ignore it by assuming it to be a trivial health complication. This leads to most cases getting diagnosed at later stages. Your esophagus is a highly sensitive organ and needs to be catered to in a precise way. Any complications that seem dangerous should be tackled by the best esophageal surgeon in your city. Never take these matters lightly or it can cost you your life.
Let us understand this issue better by diving a little deeper into esophageal cancer.
What Is Esophageal Cancer?
Esophageal cancer is a cancer affecting your food pipe (the long muscular tube connecting your throat to your stomach). It starts in the tissue of your food pipe due and spreads due to the uncontrolled division of mutated cells. In most cases, the symptoms are not noticed until the cancer reaches an advanced stage. This makes esophageal cancer one of the most dangerous and catastrophic diseases a patient can encounter.
If detected early, the tumor can be removed through surgery. If an oncologist is not able to cure a patient due to an advanced cancer stage, they do their best to make the patient live as long as possible. This is why it is important to seek immediate diagnosis and treatment for the cancer before it gets worse.
What Are The Symptoms Of Esophageal Cancer?
Most symptoms of esophageal cancer are confused with relatively smaller and harmless conditions. Here are a few common signs that should prompt you to seek serious medical help:
• Constant pain in your throat or back
• Pain behind your breastbone or between shoulders
• Coughing up or vomiting blood
• Unexplained and sudden weight loss
• A hoarse voice or cough
• Heartburn
Once developed, esophageal cancer grows at an alarming rate. Being a flexible tube, your food pipe tends to expand around the tumor as it grows, giving you a false sense of everything being alright until things get worse.
What Causes Esophageal Cancer?
What makes this cancer worse is the fact that healthcare experts have not been able to pinpoint the exact cause of the complication. However, they have identified a few major risk factors that should not be taken lightly. Here are a few such factors that can trigger esophageal cancer if not controlled:
Tobacco And Alcohol Abuse
Excessive smoking or chewing tobacco can put you at a greater risk of esophageal cancer. Excessive and prolonged drinking can also be a major contributor, worsening the condition of your food pipe.
Obesity
Being overweight can lead to esophageal inflammation, putting you at a greater risk of esophageal cancer. Make sure you watch your weight and maintain an ideal BMI to steer clear of such complications.
Barret’s Esophagus
Barret’s Esophagus refers to a condition that involves the cells lying at the lower end of your esophagus going through a change because of chronic acid reflux. If not monitored, this can lead to the formation of a cancerous tumor in your food pipe.
HPV
HPV (human papillomavirus) is a virus leading to tissue changes in your esophagus, genitals, hands, and feet. If not checked, the viral infection can lead to the development of esophageal tumor(s).
Chemical Exposure
Occupational exposure to specific chemicals for a long time can also trigger the development and spread of esophageal cancer.
Getting Esophageal Cancer Diagnosed
If you notice any of the symptoms discussed above, make sure you get yourself diagnosed without any delay. Detecting esophageal cancer at an early stage can end up saving your life. When you approach your doctor with the concern, they will conduct a brief physical examination and ask you relevant questions about your condition.
To confirm the presence of a tumor, your doctor will then ask to get one or more of the following diagnostic tests done:
Treating Esophageal Cancer
Once diagnosed, your oncologist will not waste any time and suggest the most suitable treatment procedure(s) to tackle your esophageal cancer. Here are some of the most common ways in which esophageal cancer can be treated:
The Final Word
Looking at the consequences, symptoms, and sensitivity of the condition makes it impossible to take esophageal cancer lightly. As it is rarely diagnosed at an early stage, the best you can do to stay away from esophageal cancer is to be mindful of the risk factors and take the best preventive measures under your control. Ultimately, leading a healthy life is the best (and often the only) way to keep such illnesses at bay!

18+ Yrs Exp | 5,700+ Thoracic & Robotic Cancer Surgeries
Dr. Parveen Yadav is a Director and Senior Consultant in Thoracic and Surgical Oncology, specializing in minimally invasive and robotic lung and esophageal surgeries, with advanced training from AIIMS and Tata Memorial Hospital.
View Full Profile Robotic Surgery for Esophageal Cancer in India: Benefits, Recovery and When It Is Recommended
Robotic Surgery for Esophageal Cancer in India: Benefits, Recovery and When It Is Recommended
 Best Bronchopleural Fistula Treatment in Gurgaon: What to Look for in a Thoracic Surgeon
Best Bronchopleural Fistula Treatment in Gurgaon: What to Look for in a Thoracic Surgeon
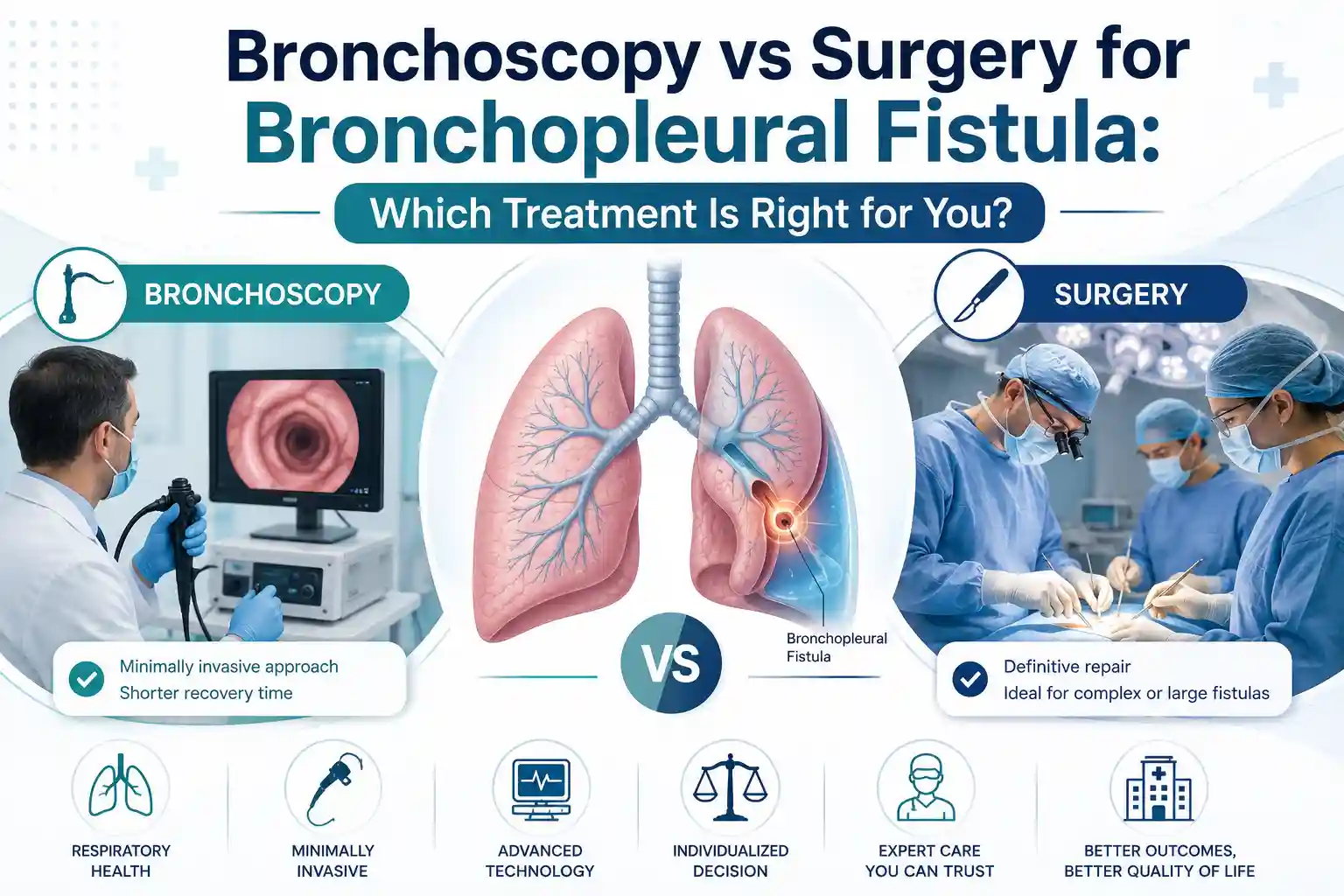 Bronchoscopy vs Surgery for Bronchopleural Fistula: Which Treatment Is Right for You?
Bronchoscopy vs Surgery for Bronchopleural Fistula: Which Treatment Is Right for You?
Learn when robotic surgery for esophageal cancer in India is recommended, its benefits, recovery, and how to consult an expert in Gurgaon.
Choosing the best bronchopleural fistula treatment in Gurgaon? Here is what to look for in a thoracic surgeon, hospital, and care team before you decide.
Bronchoscopy or surgery for bronchopleural fistula? Compare both options, success rates, recovery, and costs. Expert guidance from Dr. Parveen Yadav, Gurgaon.
Copyright 2026 © Dr .Parveen Yadav all rights reserved.
Proudly Scaled by Public Media Solution!