

Tracheal cancer is a rare type of cancer that affects the trachea or windpipe, which is essential for carrying air to and from the lungs. Despite its rarity, early detection can significantly influence the prognosis and treatment outcomes. This blog post explains the early signs of tracheal cancer, providing essential insights to raise awareness and promote early diagnosis, especially for those seeking care in regions like Gurgaon and Delhi.
Tracheal cancer originates in the trachea, the tube that joints the mouth and nose to the lungs. Although it is less common than other cancers, its impact can be severe, affecting breathing and quality of life. The trachea's role in air passage makes understanding and identifying early signs crucial for effective management.
Identifying the early signs of tracheal cancer is challenging due to their commonality with other less severe respiratory conditions. However, awareness of these symptoms can lead to earlier diagnostic efforts and better outcomes, particularly with the advanced healthcare facilities available in regions like Gurgaon and Delhi.
1. Persistent Cough
A persistent cough that doesn't resolve with standard treatments can be one of the first signs of tracheal cancer. This symptom may initially resemble a common cold but persists longer than expected, necessitating a consultation with a tracheal cancer specialist in Gurgaon, Delhi.
2. Breathing Difficulties
As the trachea narrows due to the tumour, you may experience wheezing or shortness of breath, particularly during physical activities. This symptom often progresses as the disease develops, underscoring the need for prompt medical attention at a renowned tracheal cancer hospital in Gurgaon, Delhi.
3. Voice Changes
Hoarseness or a change in the voice can occur if the cancer affects the nerves that control the vocal cords. This sign should prompt immediate consultation with healthcare providers, such as the best doctor for tracheal cancer in Gurgaon, Delhi.
4. Pain or Discomfort
If you experience pain in your throat, chest, or back, it could be a sign of advanced tracheal cancer. This pain may be constant or only occur when you cough or take deep breaths. It is essential to seek comprehensive medical care, which may include tracheal cancer surgery in Gurgaon or Delhi.
5. Recurring Respiratory Infections
Frequent respiratory infections like bronchitis or pneumonia may be a red flag for tracheal cancer. These occur because the tumour blocks the airway and traps lung bacteria. Effective treatment for such symptoms is available at leading medical institutions in Gurgaon and Delhi.
Understanding the risk factors associated with tracheal cancer is essential for prevention. These include prolonged exposure to tobacco smoke, inhalation of certain toxic chemicals, and a history of respiratory diseases. Limiting exposure to these risk factors, especially in urban areas like Gurgaon and Delhi, can help reduce the likelihood of developing tracheal cancer.
Early detection of tracheal cancer involves imaging tests such as X-rays, CT scans, MRIs, and biopsy procedures. During a biopsy, a small tissue sample is examined for cancer cells. Hospitals in Gurgaon, Delhi, are equipped with state-of-the-art facilities, which play a crucial role in the timely identification and treatment of tracheal cancer.
The treatment for tracheal cancer involves different options, such as surgery, radiation therapy, and chemotherapy. The selection of treatment depends on the stage of cancer at the time of diagnosis, as well as the patient's general health condition. Combining these treatments may sometimes be necessary to achieve the best possible outcome. Many patients have benefited from advanced surgical options and therapies in Gurgaon and Delhi.
Managing life with tracheal cancer involves adjusting to new limitations and challenges. Support from healthcare providers, family, and cancer support groups can provide the necessary assistance and improve the quality of life. The comprehensive care frameworks in Gurgaon, Delhi, ensure patients receive holistic support throughout their treatment.
Recognizing the early signs of tracheal cancer can lead to timely and potentially life-saving treatments. Dr. Parveen Yadav, a renowned expert in chest surgeries and tracheal conditions affiliated with Chest Surgery India, emphasizes the importance of early diagnosis and personalized care plans. For those experiencing persistent respiratory symptoms, consulting with specialists like Dr. Yadav can provide the expertise to manage and treat tracheal cancer effectively.
1. What are the most common early signs of tracheal cancer?
The most common early signs include a persistent cough, breathing difficulties, and changes in the voice or hoarseness.
2. How does tracheal cancer affect breathing in its initial stages?
In its initial stages, tracheal cancer can cause wheezing, shortness of breath, and general difficulty in breathing due to the narrowing of the trachea.
3. Can tracheal cancer cause changes in voice or hoarseness?
Yes, tracheal cancer can cause hoarseness or changes in voice, primarily if the tumour affects the nerves controlling the vocal cords.
4. What symptoms of tracheal cancer are often mistaken for other conditions?
Symptoms like persistent cough, recurrent respiratory infections, and hoarseness are often mistaken for less severe respiratory conditions like bronchitis or a common cold.
5. Are coughing up blood or bloody sputum early indicators of tracheal cancer?
Yes, coughing up blood or bloody sputum can be early indicators of tracheal cancer, signalling advanced irritation or damage to the trachea.
6. How early can tracheal cancer be detected?
Tracheal cancer can be detected early through imaging tests and biopsies, uncommonly if symptoms prompt an early evaluation.
Dr. Parveen Yadav is a highly recommended surgeon or specialist for Tracheal cancer treatment in Gurgaon, Delhi. He specialises in minimally invasive and robotic thoracic onco surgery. He has been recognised for 17+ years as the best chest surgeon in Gurgaon, Delhi, for his expertise in treating chest-related (Chest Surgery) ailments, such as Esophageal (Food Pipe Cancer), Lung, Tracheal (Throat), Chest wall tumours, Mediastinal Tumors, Empyema, and Bronchopleural Fistula cancer. With a focus on precision and innovation, he is dedicated to offering exceptional care to his patients, utilising advanced techniques to ensure optimal outcomes.

18+ Yrs Exp | 5,700+ Thoracic & Robotic Cancer Surgeries
Dr. Parveen Yadav is a Director and Senior Consultant in Thoracic and Surgical Oncology, specializing in minimally invasive and robotic lung and esophageal surgeries, with advanced training from AIIMS and Tata Memorial Hospital.
View Full Profile Best Bronchopleural Fistula Treatment in Gurgaon: What to Look for in a Thoracic Surgeon
Best Bronchopleural Fistula Treatment in Gurgaon: What to Look for in a Thoracic Surgeon
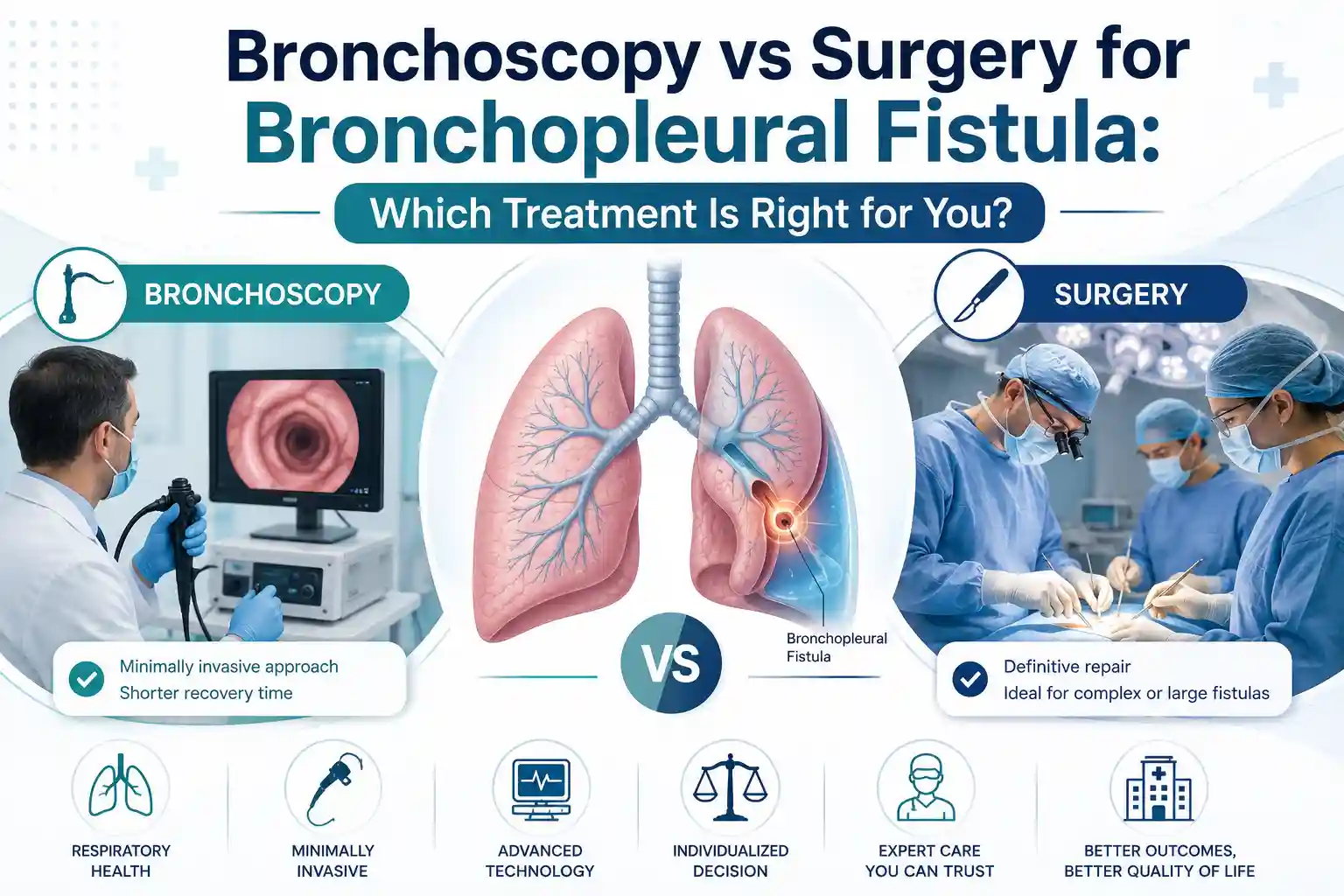 Bronchoscopy vs Surgery for Bronchopleural Fistula: Which Treatment Is Right for You?
Bronchoscopy vs Surgery for Bronchopleural Fistula: Which Treatment Is Right for You?
 Lung Cancer in Non-Smokers: Symptoms, Causes and When to See a Specialist
Lung Cancer in Non-Smokers: Symptoms, Causes and When to See a Specialist
Choosing the best bronchopleural fistula treatment in Gurgaon? Here is what to look for in a thoracic surgeon, hospital, and care team before you decide.
Bronchoscopy or surgery for bronchopleural fistula? Compare both options, success rates, recovery, and costs. Expert guidance from Dr. Parveen Yadav, Gurgaon.
Know the symptoms, causes, risk factors, and warning signs of lung cancer in non-smokers. Learn when to consult a lung cancer specialist in Gurgaon.
Copyright 2026 © Dr .Parveen Yadav all rights reserved.
Proudly Scaled by Public Media Solution!